Leave Your Message
Selecting the right Medical IT Isolated Power System is crucial for healthcare facilities. A well-functioning system ensures patient safety and equipment reliability. Hospitals are complex environments where electrical safety is paramount. An isolated power system minimizes the risks of electrical faults that can lead to serious consequences.
Understanding the specific needs of your facility is essential. Consider factors such as the number of patients, types of equipment, and operational requirements. Not all systems are created equal. Some may lack the necessary features for critical care environments. Engaging with experts in electrical systems can provide valuable insights. However, don’t solely rely on professional opinions; hands-on research is essential.
Evaluating different options can be challenging. One must consider the costs, installation specifics, and ongoing maintenance. The variability in quality and features requires careful scrutiny. A reliable system should offer robust performance without frequent disruptions. Investing time in this process can help prevent serious issues later on.

When choosing a medical isolated power system, understanding its key features is essential. These systems provide safety and reliability in healthcare facilities. They isolate electrical circuits from the ground, preventing potential shock hazards. Such systems are crucial in operating rooms and critical care units, where equipment must function without interruption.
It's important to consider the design and testing standards of these systems. Check if they comply with industry regulations. A reliable power system will have built-in monitoring tools. These features help detect faults or ground leaks promptly. Users should be trained to interpret these alerts effectively.
Tips: Regular maintenance checks are necessary to ensure consistent performance. Test equipment frequently to avoid unexpected failures. Document all findings and update protocols as needed. Transparency in operations fosters a culture of safety. Remember that continual improvement is vital. In a healthcare setting, every detail counts.
| Feature | Description | Importance | Considerations |
|---|---|---|---|
| Isolation Monitoring | Continuous monitoring of the isolation resistance of the system to prevent electrical shock. | Critical for patient safety. | Ensure alerts are audible and visible. |
| Ground Fault Protection | Protection against ground faults which could cause equipment damage or pose risks to patients. | Essential for electrical safety. | Verify response time and threshold settings. |
| Alarm Systems | Integrated alarm systems to signal issues with power isolation. | Vital for immediate response. | Check for redundancy and backup options. |
| Surge Protection | Protection against voltage spikes and surges to safeguard medical devices. | Prevents equipment failure. | Review device specifications for compatibility. |
| Size and Footprint | Physical dimensions and installation requirements of the power system. | Affects facility space planning. | Ensure it fits within existing space constraints. |
When selecting a medical isolated power system, several critical factors must be considered. Safety is paramount. The system should meet the standards set by organizations like the National Fire Protection Association (NFPA). In the U.S., approximately 28% of electrical fires in healthcare settings are caused by faulty wiring. A reliable power system minimizes this risk.
Next, assess the system's capacity and flexibility. Systems should adapt to different load requirements. Research indicates that facilities expect power loads to increase by 30% over the next decade. Therefore, choosing a system that can handle future demands is vital. Additionally, installation requirements and maintenance capabilities often vary. An overly complex system may lead to higher operational costs and increased downtime.
Lastly, consider the system's monitoring and alert capabilities. Real-time monitoring can prevent failures. According to a study by the American Hospital Association, outages in medical facilities can cost around $1.4 million annually. Systems with advanced monitoring features can enhance reliability and reduce these potential losses. Ultimately, taking these factors into account can lead to a more effective power management strategy in a healthcare environment.
When choosing a medical isolated power system, understanding industry standards is crucial. These standards ensure the safety and reliability of electrical systems in healthcare environments. Specifically, the National Fire Protection Association (NFPA) recommends adhering to NFPA 99, which outlines critical aspects of isolation transformer requirements. Compliance with these standards can significantly impact patient safety and operational efficiency.
Moreover, the Institute of Electrical and Electronics Engineers (IEEE) has established guidelines detailing the testing and maintenance of isolated power systems. A report indicates that more than 60% of healthcare facilities face electrical failures due to non-compliance with these guidelines. Regular assessments can identify issues before they escalate, emphasizing the need for a robust maintenance plan.
Another important factor is the unique requirements for equipment and surgical devices used in hospitals. These devices often require specific isolation levels to minimize risks. It’s essential to consider these specifics when selecting a system. Often, institutions overlook how poor grounding practices can lead to serious hazards. Recognizing and addressing these oversights can prevent grave accidents in medical facilities.
When selecting a medical isolated power system, evaluating performance metrics is crucial. Efficiency and reliability are two key elements that should guide decisions. According to the IEEE 516 standard, a reliable system should maintain a minimum uptime of 99.9%. This standard highlights the need for continuous monitoring to prevent downtime, which can be critical in healthcare settings.
Efficiency metrics often include energy consumption, which can impact operational costs. A report from the U.S. Department of Energy indicates that optimizing power systems can lead to a 30% reduction in energy costs over time. This is significant, especially for hospitals that operate around the clock. Regular audits can help identify inefficiencies and inform upgrades.
However, one must also consider the potential limitations of isolated power systems. Not all systems provide equal protection; some may lack features necessary for specific medical environments. It’s essential to weigh these factors against the benefits. Seeking expert advice can offer valuable insights. Engaging with professionals ensures that choices align with the unique needs of your facility.
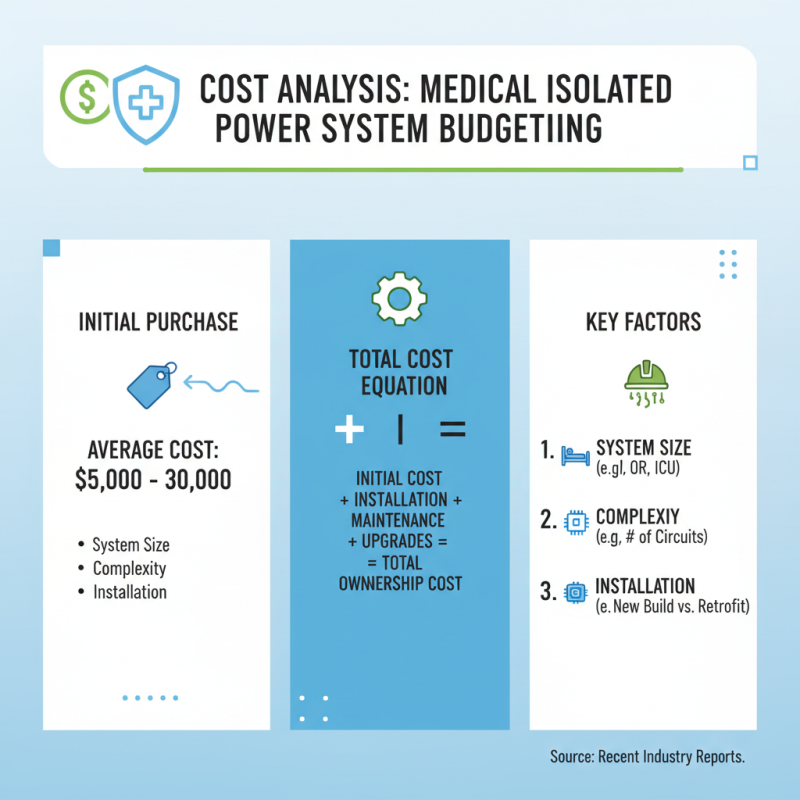
When budgeting for a medical isolated power system, understanding costs is critical. The initial purchase is just one part of the equation. According to recent industry reports, the average cost of these systems can range from $5,000 to $30,000. Factors affecting this range include system size, complexity, and installation requirements.
Ongoing maintenance and operational costs must also be considered. Statistical data indicates that maintenance can account for 10-20% of overall system costs annually. Regular inspections and repairs are essential to ensure system reliability and longevity. Facilities might choose to invest in training for staff, which can lead to extra expenses but ultimately improves safety and compliance.
Additionally, energy efficiency plays a crucial role in long-term budgeting. Systems that optimize energy use can reduce operational costs significantly over time. However, the upfront investment in energy-efficient technologies can be daunting. This reflects a balancing act between short-term expenditure and long-term savings, prompting many facilities to rethink their budget allocations.






